 By Beth Onofri, Clinical Market Advisor, Kareo
By Beth Onofri, Clinical Market Advisor, Kareo
Twitter: @GoKareo
In October 2016 the final MACRA rule was released. The rule laid out the Quality Payment Program (QPP) which consolidates previous CMS incentive programs into a single program that began on January 1, 2017. The QPP has two possible paths for eligible clinicians. The Merit-Based Incentive Payment System (MIPS) is the path that most providers will take in 2017. It is comprised of three categories. Each category represents a portion of a total composite score of 100%. The potential penalties and incentives for MIPS are based on the total composite score. Eligible clinicians (EC) may receive anywhere from a -4% adjustment to a +12% adjustment. Here is an overview of the Quality category, which replaces the PQRS program.
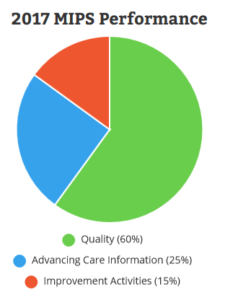
The Quality category represents the largest portion of the total composite score at 60%. The Quality category requires a minimum of six quality measures, including an outcome measure. ECs must use a certified EHR to participate and report on all patients.
There are 271 total measures to choose from, and they can be sorted by specialty. They can also be sorted by high priority. This will get you the outcomes measures and high priority measures. If there isn’t an outcomes measure suitable to your specialty, you can choose another high priority measure instead.
For those who want to be high achievers and potentially get the added incentive, do more than six measures. For example, if you already do nine measures for PQRS then keep doing those nine.
The reporting period is January 2, 2018 through March 31, 2018, and the Quality measures can be reported through:
- Claims (individual only)
- Qualified Registry
However, CMS strongly advises against claims reporting since you must use a certified EHR to collect the data. If you use claims reporting then you have to enter and track the data in your EHR, run the necessary reports, and then report the data through your claims. This would be more work than using the qualified registry.
This article was originally published on Kareo’s Go Practice Blog and is republished here with permission.
