Shared Savings Program ACOs Saved $4.1 Billion in 2020
Medicare’s largest alternative payment model produced its highest annual savings to date in 2020, while continuing to provide high-quality care, as shown by performance data released by the Centers for Medicare & Medicaid Services (CMS).
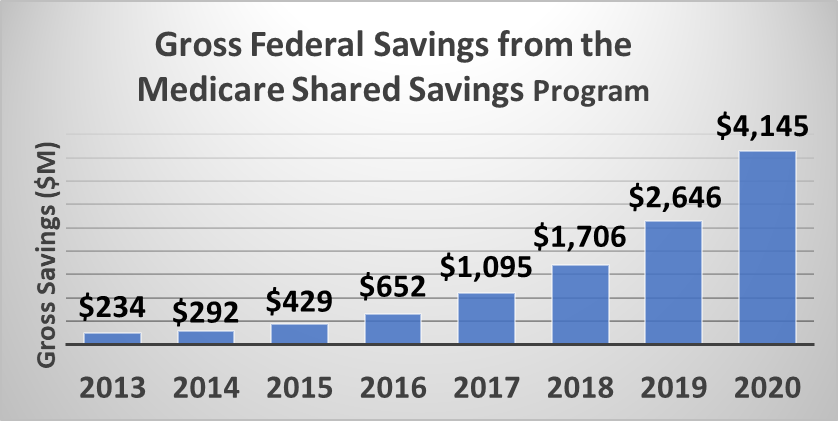
The Medicare Shared Savings Program, the accountable care organization (ACO) model that served 10.6 million seniors in 2020, collectively saved Medicare $4.1 billion last year, and $1.9 billion after accounting for shared savings payments. Importantly, these ACOs also hit an average quality score of 97.8 percent and 60 ACOs earned a perfect score of 100. This is an improvement over the $2.6 billion and $1.2 billion in gross and net savings MSSP created in 2019, making 2020 the best year yet for ACOs.
“This data underscores the need for policymakers to do all they can to grow the ACO model and extend the program’s benefits to more patients,” said Clif Gaus, Sc.D., president and CEO of the National Association of ACOs (NAACOS) (@NAACOSnews). “We currently have the fewest number of Shared Savings Program ACOs since 2017. That trend must be reversed, given continued debate about ways to improve our health system.”
ACOs provide an alternative to the fragmented fee-for-service system by holding groups of doctors, hospitals, and other providers who come together accountable for the cost and quality of a defined set of patients. They earn the right to share with Medicare savings generated if certain spending and quality metrics are met. Results for all 2020 Shared Savings Program ACOs, which compare the year’s spending to pre-set targets, are available in an online public use data file. In 2020, 513 ACOs participated in the Shared Savings Program, whose participation is voluntary.
NAACOS attributes the drop in ACOs to several Trump-era policies, including 2018 changes CMS called “Pathways to Success,” which gave ACOs limited time before taking on financial risk and cut the share of savings most ACOs are eligible to keep. NAACOS supports the Value in Health Care Act (H.R. 4587), which would increase shared savings rates, create favorable risk adjustment and benchmarking policies, and provide at least three years before being forced to take on risk. We and other leading healthcare organizations are pushing Congress to include the Value Act in the upcoming reconciliation bill.
Other key points from the ACO results:
- $390 in gross savings per beneficiary
- 345 out of 513, or 67 percent, of ACOs earned shared savings
- ACOs earned $2.3 billion in shared savings payments
- 75 percent of shared savings-only ACOs produced gross savings and 55 percent earned shared savings
- 97 percent of at-risk ACOS produced gross savings and 88 percent earned shared savings
During the pandemic-stricken year of 2020, ACOs were valuable assets in managing patient care. Given their accountability to long-term patient care and outcomes, ACOs were proactive in their outreach to high-risk patients to keep them healthy, quickly established telehealth and remote monitoring capabilities to continue to provide care, and effectively managed home visits and post-acute care to reduce COVID transmission.
In addition to the positive 2020 results, multiple analyses have shown ACOs are lowering Medicare spending by 1 percent to 2 percent, which translates into tens of billions of dollars of reduced Medicare spending when compounded annually.
About NAACOS
The National Association of ACOs (NAACOS) represents more than 12 million beneficiary lives through hundreds of organizations participating in population health-focused payment and delivery models in Medicare, Medicaid, and commercial insurance. Models include the Medicare Shared Savings Program (MSSP), Next Generation ACOs, and alternative payment models supported by a myriad of commercial health plans and Medicare Advantage. NAACOS is a member-led and member-owned nonprofit organization that works to improve quality of care, outcomes, and healthcare cost efficiency.
